Anophthalmos
Surgical and prosthetic management of anophthalmos (absence of the eye) and socket reconstruction following enucleation or evisceration.
Anophthalmos — Overview
Anophthalmos (or anophthalmia) refers to the absence or loss of the eye within the orbit. The term covers a broad spectrum: from congenital absence of the globe, to acquired loss of the eye due to trauma, tumor, or advanced ocular disease. Regardless of the cause, the result is an empty or shrunken socket that requires reconstruction to restore volume, support a prosthesis, and maintain a normal facial appearance.
Modern orbital implants and socket reconstruction techniques have transformed outcomes for patients with anophthalmos. Dr. Brown provides orbital implant surgery, socket reconstruction, and long-term prosthetic management for patients of all ages, including children with congenital conditions requiring stimulation of orbital growth.
Classifications of Anophthalmos
Congenital anophthalmos is classified by the stage at which ocular development failed:
- Primary anophthalmia is a complete absence of eye tissue due to failure of the optic vesicle to form from the developing brain.
- Secondary anophthalmia occurs when the eye begins to develop but stops at an early stage, leaving only residual ocular tissue or extremely small eyes visible only on close examination.
- Degenerative anophthalmia occurs when a partially formed eye undergoes regression, often attributed to a disruption in blood supply during fetal development.
True primary anophthalmos is very rare; extreme microphthalmos (a very small globe within the orbital soft tissue) is more commonly encountered clinically. Anophthalmos and microphthalmos can occur as isolated findings or as part of syndromes associated with chromosomal abnormalities, including Trisomy 13.
Causes of Anophthalmos
Congenital anophthalmos may result from inherited or sporadic genetic mutations, chromosome abnormalities, prenatal environmental insults (infections, teratogens), or unknown causes. Development of the eyelids, conjunctival fornices, and bony orbit is dependent on the presence of a normal-sized eye during fetal growth; absence or severe reduction of the globe impairs orbital development and requires early intervention.
Acquired anophthalmos results from surgical removal of the eye due to:
- Trauma (severe ocular injury not amenable to repair)
- Tumor (retinoblastoma, choroidal melanoma, other intraocular malignancies)
- Infection (endophthalmitis unresponsive to treatment)
- Advanced ocular disease (end-stage glaucoma, painful blind eye from corneal or uveal disease)
Surgical Options — Evisceration & Enucleation
When the eye cannot be saved, two primary surgical procedures are available:
- Evisceration — removal of the intraocular contents while preserving the scleral shell. The sclera and extraocular muscles remain intact, which provides excellent implant motility. Evisceration is generally preferred when there is no concern for intraocular malignancy, as it preserves more tissue and may result in better prosthetic movement. It carries a small theoretical risk of sympathetic ophthalmia.
- Enucleation — removal of the entire globe, including the sclera, leaving the extraocular muscles and orbital fat. Enucleation is required when intraocular malignancy is present or suspected. After enucleation, the extraocular muscles are sutured to the orbital implant to restore movement.
Following either procedure, an orbital implant is placed within the muscle cone to restore orbital volume. A custom ocular prosthesis is fitted by an ocularist 4–6 weeks after surgery.
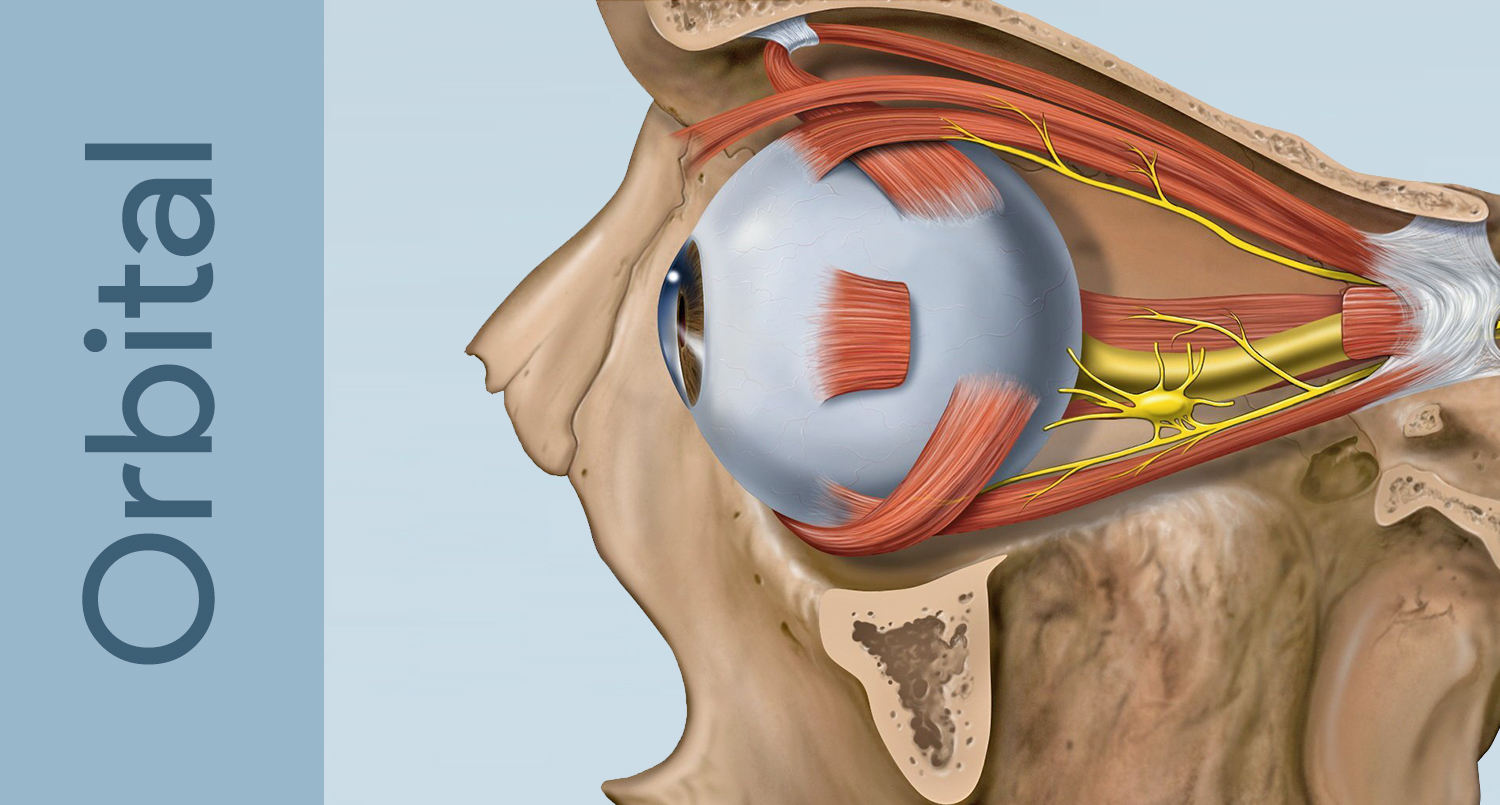
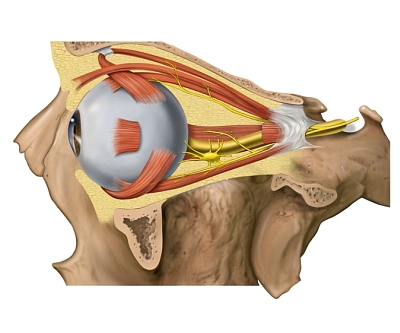
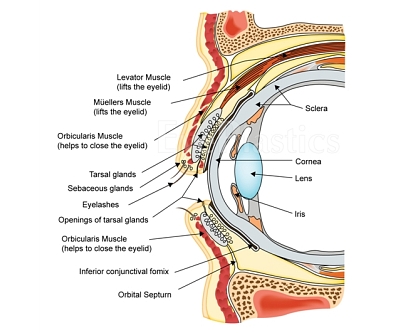
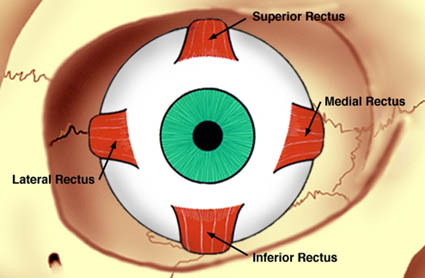
Anophthalmos — Evisceration & Enucleation Animation
Interactive animation covering ocular anatomy and the surgical procedures of evisceration and enucleation.
Orbital Implants
The choice of implant material and design affects vascularization, motility, implant stability, and long-term outcomes. Modern porous implants allow fibrovascular ingrowth, which anchors the implant and reduces the risk of migration and extrusion.
MEDPOR® (Porous Polyethylene)
MEDPOR® is a lightweight, porous high-density polyethylene with an extensive interconnecting pore structure. Its porosity allows rapid fibrovascular ingrowth, integrating the implant into the patient’s own tissues. Available in spheres (14–22 mm diameter) and custom shapes. The Conical Orbital Implant (COI)® variant includes channels for rectus muscle attachment and a superior projection to reduce the post-operative superior sulcus defect.
Hydroxyapatite (HA)
The coralline hydroxyapatite implant is a spherical implant composed of natural calcium phosphate hydroxide, the same mineral found in human bone. Its porous structure supports fibrovascular ingrowth and direct attachment of extraocular muscles. Historically the most widely used porous implant, HA implants provide excellent motility and low extrusion rates compared to older nonporous synthetic materials.
Bioceramic (Alumina)
Bioceramic implants are made of porous alumina (Al&sub2;O&sub3;) with highly uniform interconnected pores (~500 µm). The extensive pore system enhances fibrovascular ingrowth and secure muscle attachment. The material is strong, non-brittle, and biocompatible.
Dermis-Fat Graft
A dermis-fat graft uses a disc of the patient’s own dermis and subcutaneous fat, typically harvested from the lower abdomen or outer quadrant of the buttock. As an autologous graft, it eliminates concerns about biocompatibility and disease transmission. The graft can grow in children, providing ongoing stimulus for orbital development — a significant advantage over fixed-size implants in early childhood.
Indications for dermis-fat graft include:
- Primary socket reconstruction in young children where orbital growth stimulation is needed
- Replacement of an extruded or infected orbital implant
- Correction of post-enucleation superior sulcus deformity (volume deficit)
- Orbital exenteration reconstruction
The graft is measured approximately 25 mm in diameter; the dermis is often shaped into a dome to improve prosthesis motility. Potential complications include fat atrophy (leading to some volume unpredictability), central graft ulceration, cyst or granuloma formation, and donor site morbidity.
Complications & Socket Management

Post-enucleation socket syndrome results from volume loss and structural changes after globe removal. The 7 ml of volume lost when the eye is removed is only partially replaced by standard implants (an 18 mm sphere provides ~3 ml; a 20 mm sphere ~4.1 ml), compounded by up to 3 ml of orbital fat atrophy over time. Manifestations include:
- Enophthalmos — posterior displacement of the implant/prosthesis
- Deep superior sulcus — hollowing above the upper eyelid from volume loss
- Lower eyelid laxity — with shallow fornix and loss of fornix depth, making prosthesis retention difficult
- Ptosis or lid retraction — from changes in the levator complex
Implant Exposure and Extrusion
Implant exposure — a breakdown in the conjunctival covering over the implant — is the most common serious complication. A small exposure may be repaired surgically with a patch graft. Larger exposures or progressive extrusion may require implant removal and replacement, often with a dermis-fat graft. Early recognition and treatment prevents implant loss.
Other Complications
- Hemorrhage — more common in patients on anticoagulants; usually managed conservatively with analgesics
- Infection — rare with modern porous implants; most secondary infections respond to antibiotics; severe cases may require implant removal
- Poorly fitting prosthesis — socket changes over time alter the fit of the ocular prosthesis; regular ocularist visits (every 1–2 years) are recommended for polishing, refitting, and replacement as needed
Schedule a Consultation
Contact us to discuss your concerns and learn about treatment options.