Lagophthalmos
Treatment of lagophthalmos — incomplete eyelid closure from facial nerve palsy or Bell's palsy — to protect the cornea and restore function.
Lagophthalmos
Lagophthalmos is incomplete or absent closure of the eyelids. When the eyelid cannot fully close, the cornea and conjunctiva are exposed to evaporation, drying, and trauma — leading to exposure keratopathy that can progress from punctate erosions to corneal ulceration, scarring, and permanent vision loss.
The severity of corneal exposure depends on three factors: the degree of lagophthalmos (how many millimeters the eye fails to close), the blink rate (which spreads the tear film), and the quality of tear film (lubrication). Bell’s phenomenon — the normal reflex that rotates the eye upward on attempted closure — provides some protection, but its presence does not eliminate exposure risk.
For a detailed guide to eyelid anatomy, see our dedicated Eyelid Anatomy page.
Causes
Lagophthalmos results from either neuromuscular failure of eyelid closure or mechanical restriction that prevents closure despite intact muscle function.
Facial Nerve Palsy (CN VII)
Facial nerve palsy is the most common cause. The facial nerve supplies the orbicularis oculi muscle — the muscle that closes the eyelid. Paralysis produces lagophthalmos (failed closure), ectropion (lower lid sag), brow ptosis, and loss of the normal blink reflex.
- Bell’s palsy — idiopathic peripheral CN VII palsy; accounts for ≈ 70% of cases; most recover within 6 months but 15–30% have some residual weakness
- Herpes zoster oticus (Ramsay Hunt syndrome) — VZV reactivation in the geniculate ganglion; recovery less complete than Bell’s; associated with ear vesicles and hearing loss
- Trauma — temporal bone fractures, facial lacerations, or iatrogenic (parotid surgery, acoustic neuroma resection)
- Tumors — parotid gland tumors, acoustic neuromas, cerebellopontine angle masses, and cholesteatoma
- Central lesions — stroke, multiple sclerosis; upper motor neuron lesions spare forehead muscles (bilateral cortical representation)
- Lyme disease — bilateral CN VII palsy is characteristic of Lyme neuroborreliosis
- Möbius syndrome — congenital bilateral CN VI and CN VII palsy
Non-Neurogenic Causes
- Thyroid eye disease (Graves’) — upper lid retraction prevents full descent and contact with the lower lid
- Proptosis (any cause) — the globe projects beyond the orbital rim; the lids cannot close over it
- Cicatricial lagophthalmos — scarring of the anterior lamella (skin and orbicularis) from burns, trauma, previous surgery, or Stevens-Johnson syndrome shortens the vertical dimension and prevents closure
- Nocturnal lagophthalmos — incomplete closure during sleep; often idiopathic; patients are unaware but wake with dry, irritated eyes
Evaluation
Clinical evaluation quantifies the degree of exposure and assesses corneal risk:
- Lagophthalmos measurement — the gap between lids on gentle and forced closure, in millimeters. Gentle closure simulates physiological blink; forced closure indicates the reserve available for corneal protection
- Bell’s phenomenon — the eyeball rotates upward on attempted closure, positioning the cornea under the upper lid; protects against exposure in many patients
- Corneal sensation — patients with herpes zoster or acoustic neuroma often have coincident CN V (trigeminal) involvement, which reduces corneal sensation and dramatically increases ulceration risk (neurotrophic keratopathy)
- Slit-lamp examination — documents punctate keratopathy (inferior cornea), epithelial erosions, infiltrates, or ulceration
- Schirmer test / tear film assessment — concurrent dry eye markedly worsens exposure risk
- Lower eyelid position — facial nerve palsy often causes concurrent lower lid ectropion, which reduces lacrimal pump function and opens the inferior conjunctival fornix to air
Treatment
Treatment is stratified by the severity of lagophthalmos, the expected duration (temporary vs. permanent palsy), and the degree of corneal compromise. The goal is to restore a functional tear film over the entire corneal surface with every blink.
Medical Management (First Line)
All patients with lagophthalmos require lubrication therapy. The protocol is escalated based on severity:
- Preservative-free artificial tears — every 1–2 hours while awake; preservatives cause corneal toxicity with frequent dosing
- Lubricating ointment at bedtime — longer residence time; essential for nocturnal exposure; blurs vision so used only during sleep
- Moisture chamber — a humid microenvironment over the eye (tape, swim goggles, or specialized chambers) reduces evaporative tear loss; most effective for nocturnal lagophthalmos
- Eyelid taping — medical-grade tape applied vertically over the closed lid at night; simple and effective for temporary palsy; avoid skin irritation
- Scleral contact lens — creates a liquid reservoir over the cornea; used for severe keratopathy when surgery is deferred
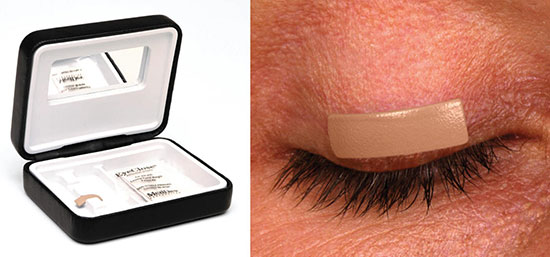
External Eyelid Weights (Temporary)
External gold or platinum weights (0.6–2.0 g) can be taped to the pretarsal skin of the upper lid to supplement lid descent. They are used to identify the optimal weight before implantation, to test patient tolerance, and as a temporizing measure while awaiting nerve recovery. They are not practical for long-term use.
Surgical Management
Surgery is indicated when medical management fails to prevent corneal progression or when the lagophthalmos is expected to be permanent. The timing is individualized — for Bell’s palsy, most surgeons wait 6–12 months for potential spontaneous recovery before committing to permanent procedures.
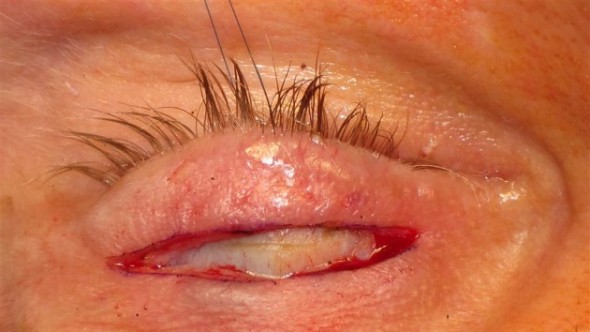
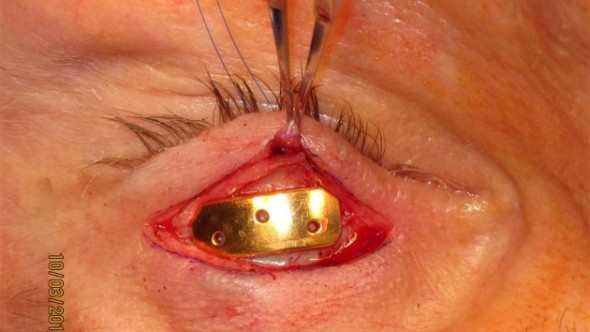
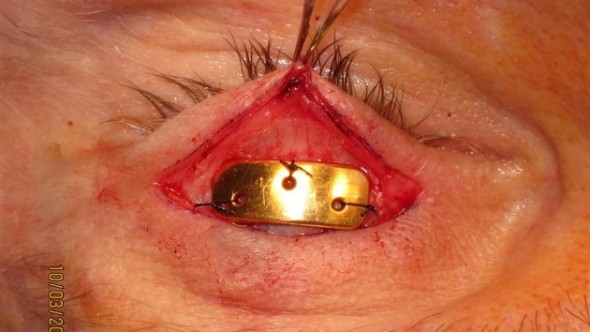
Gold Weight Implantation (Upper Lid Loading)
Gold weight implantation is the most commonly performed procedure for paralytic lagophthalmos. A precisely calibrated weight (gold or platinum, 0.6–2.0 g — selected by preoperative external weight testing) is placed in the pretarsal space of the upper eyelid through a lid-crease incision. The weight augments gravity-assisted lid descent; as the patient relaxes the levator, the weight closes the lid.
- Highly effective for daytime closure; less effective for nocturnal lagophthalmos (patient supine, gravity less helpful)
- Reversible — the weight can be removed or exchanged if function recovers or weight selection was suboptimal
- Complications include implant migration (1–5%), visibility through thin lid skin, and ptosis if overly heavy
- Platinum is used in patients with known gold allergy and has a smaller profile for equivalent weight
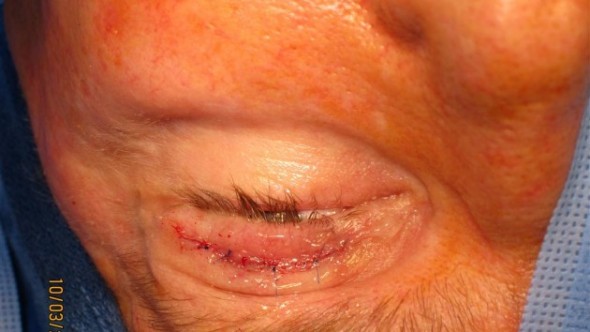
Tarsorrhaphy
Tarsorrhaphy narrows the palpebral fissure by suturing the upper and lower lid margins together at the lateral canthus (lateral tarsorrhaphy) or, rarely, medially. It is the most durable and reliable procedure for corneal protection but is the most visually and cosmetically disruptive.
- Lateral tarsorrhaphy — closes 3–8 mm of the lateral fissure; reduces the exposed corneal area without obstructing the visual axis; can be performed under local anesthesia
- Temporary tarsorrhaphy — sutures placed without tissue excision; reversible when the palsy resolves
- Permanent tarsorrhaphy — includes excision of a strip of lid margin to create a durable adhesion; used for permanent lagophthalmos
- Indicated when gold weight is insufficient, when Bell’s phenomenon is absent, or when lagophthalmos is combined with severe dry eye or neurotrophic keratopathy
Lower Eyelid Procedures
Facial nerve palsy often produces concurrent lower lid ectropion and scleral show that worsens exposure. Lower lid procedures may be combined with upper lid loading:
- Canthoplasty / canthopexy — tightens the lower lid canthal tendon to elevate and support the lower lid margin
- Lower lid spacer graft — hard palate or acellular dermis grafted to the posterior lamella to raise the lower lid margin and reduce inferior scleral show
- Midface lift — corrects malar descent that contributes to lower lid sagging in long-standing palsy
Managing the Paralytic Lower Lid
In severe or long-standing facial nerve palsy, the lower lid undergoes progressive ectropion and descent due to orbicularis weakness, gravity, and denervation atrophy of the midface. This creates a wide palpebral fissure that cannot be fully protected by upper lid procedures alone. A comprehensive treatment plan typically addresses both lids: upper lid weight or spring implant for closure, and lower lid canthoplasty or spacer graft for support.
Schedule a Consultation
Contact us to discuss your concerns and learn about treatment options.
Related Conditions
Eyelid Laxity
Treatment of lax or loose eyelids — ectropion, entropion, floppy eyelid syndrome — causing discomfort, tearing, or corneal exposure.
Learn more →Blepharoplasty
Upper and lower eyelid blepharoplasty ("eye lift") — cosmetic and functional correction of excess eyelid skin and fat.
Learn more →

