Skin Tumors
Diagnosis and surgical removal of benign and malignant eyelid skin tumors with reconstruction — including basal cell, squamous cell, and melanoma.
Eyelid Skin Tumors
The eyelid is one of the most common sites for skin tumors on the body, both benign and malignant. Because the eyelid protects the eye, even small tumors in this location have functional and aesthetic significance. Dr. Brown evaluates, biopsies, removes, and reconstructs eyelid tumors as a single-surgeon team — a key advantage when Mohs surgery and oculoplastic reconstruction must be coordinated on the same day.
The first step with any new eyelid lesion is accurate diagnosis. Clinical features, growth rate, and patient history guide whether a lesion needs observation, office biopsy, or excision. When cancer is suspected, margin-controlled excision (Mohs micrographic surgery or frozen-section control) is standard of care before reconstruction.
Benign Eyelid Lesions
Most eyelid lesions are benign. They are grouped by tissue of origin — epithelial, glandular, vascular, and inflammatory. The key clinical task is distinguishing benign from pre-malignant or malignant lesions, which can look deceptively similar.
Epithelial Lesions
Squamous papilloma (skin tag) is the most common benign eyelid lesion — a soft, pedunculated or sessile growth arising from the epidermis, often at the lid margin or medial canthus. It is caused by HPV and is treated by snip excision.
Seborrheic keratosis appears as a waxy, “stuck-on” brown plaque with a velvety or verrucous surface. It is benign and may be observed; excision or cryotherapy is performed if symptomatic or cosmetically bothersome.
Keratoacanthoma is a rapidly growing, cup-shaped nodule with a central keratin plug that appears over weeks, then may involute. Because it can be clinically indistinguishable from squamous cell carcinoma, excision with pathologic confirmation is required.
Actinic keratosis is a pre-malignant epithelial lesion caused by cumulative UV damage. It appears as a rough, erythematous, scaly patch on sun-exposed skin. Untreated, ~1–5% progress to squamous cell carcinoma annually. Treatment is excision or cryotherapy.
Cysts
Epidermal inclusion cysts are smooth, firm, skin-colored nodules formed by trapped keratinizing epithelium. They are the most common eyelid cysts and are treated by complete excision of the cyst wall.
Dermoid cysts are congenital choristomas containing hair follicles and adnexal structures. They classically occur at the supero-temporal orbital rim (frontozygomatic suture) or supero-medially. Dermoids do not involute and are excised electively — rupture causes severe granulomatous inflammation.
Sweat ductal cysts (eccrine or apocrine hidrocystomas) appear as translucent, fluid-filled cysts along the lid margin. They may enlarge in warm weather. Marsupialization or excision is curative.
Vascular Lesions
Capillary hemangioma (infantile hemangioma) is the most common orbital and periorbital tumor of childhood. It proliferates rapidly in the first year of life, then slowly involutes by age 7. If the lesion causes amblyopia, astigmatism, or significant ptosis, early treatment with oral propranolol is indicated.
Port-wine stain (nevus flammeus) is a vascular malformation present at birth and does not involute. Extensive port-wine stains in the V1 distribution may be associated with Sturge-Weber syndrome and require glaucoma screening. Pulsed-dye laser is the primary treatment.
Pyogenic granuloma appears as a rapidly growing, red, bleeding vascular nodule, typically after minor trauma or surgery. Despite the name, it is not infectious. Treatment is excision.
Pigmented Lesions (Nevi)
Eyelid nevi may be junctional, compound, or intradermal. A lid margin nevus is common and often stable for years. Indications for excision include change in size, shape, color, or bleeding — all of which raise concern for melanoma. The nevus of Ota (oculodermal melanocytosis) involves periocular skin and the episclera and carries a small risk of uveal melanoma; ophthalmologic follow-up is recommended.
Chalazion
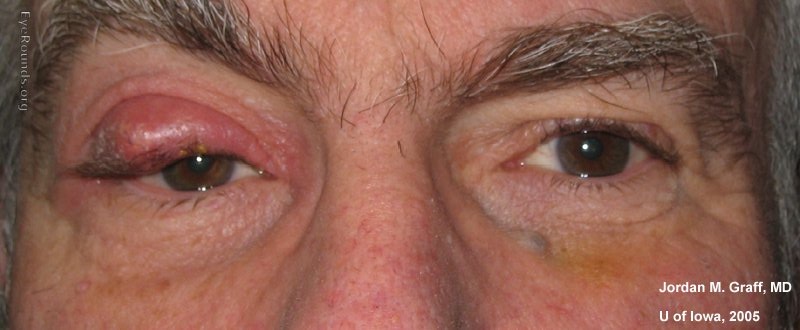
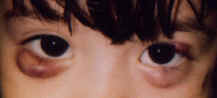
A chalazion is a sterile lipogranulomatous inflammatory lesion of the eyelid, caused by obstruction of a meibomian gland duct with retained secretions. It differs from a hordeolum (stye) in that it is not primarily infectious, though secondary infection can occur.
Natural history: The majority of chalazia resolve spontaneously or with conservative management within 4–6 weeks. Warm compresses (5–10 minutes, 4 times daily) soften meibomian secretions and facilitate drainage. Gentle lid massage after warming helps evacuate the obstructed gland. Topical antibiotic/steroid drops are used if there is associated blepharitis or early infection.
Intralesional steroid injection (triamcinolone acetonide 5–10 mg/mL, 0.1–0.2 mL) is effective for chalazia that fail conservative treatment, achieving resolution in 60–80% of cases. A single injection may be repeated once. Complications include skin depigmentation — particularly important to counsel in patients with darker skin tones.
Incision and curettage (I&C) is performed under local anesthesia when the lesion has been present >6 weeks without improvement. A small vertical incision is made on the inner (tarsal) surface of the lid to avoid a visible scar, and the granulomatous material is curetted out. Recovery is rapid and the success rate is >90%.
Any chalazion that recurs after proper treatment, or that is firm, fixed, or has irregular margins, should be sent for pathologic examination to exclude sebaceous gland carcinoma, which can perfectly mimic a chalazion.
Xanthelasma

Xanthelasma palpebrarum are yellowish, soft plaques of lipid-laden macrophages (foam cells) deposited in the superficial dermis of the medial eyelids. They are the most common form of cutaneous xanthoma. Approximately 50% of patients with xanthelasma have an underlying lipid disorder (hypercholesterolemia, hypertriglyceridemia, or mixed dyslipidemia) — fasting lipid panel and cardiovascular risk assessment are appropriate at initial evaluation.
Xanthelasma is benign and carries no risk of malignant transformation. Indications for treatment are cosmetic. Options include:
- Surgical excision — most reliable for localized lesions; risk of ectropion if large areas are removed near the lid margin
- Trichloroacetic acid (TCA) chemical ablation — 70–100% TCA applied with a fine applicator; multiple treatments often needed
- CO2 or Er:YAG laser ablation — precise depth control; effective for thin, superficial lesions
- Cryotherapy — less commonly used due to risk of hypopigmentation
Recurrence is common regardless of treatment modality, especially if the underlying dyslipidemia is not controlled. Statin therapy or dietary modification may slow recurrence but does not reliably cause regression.
Molluscum Contagiosum
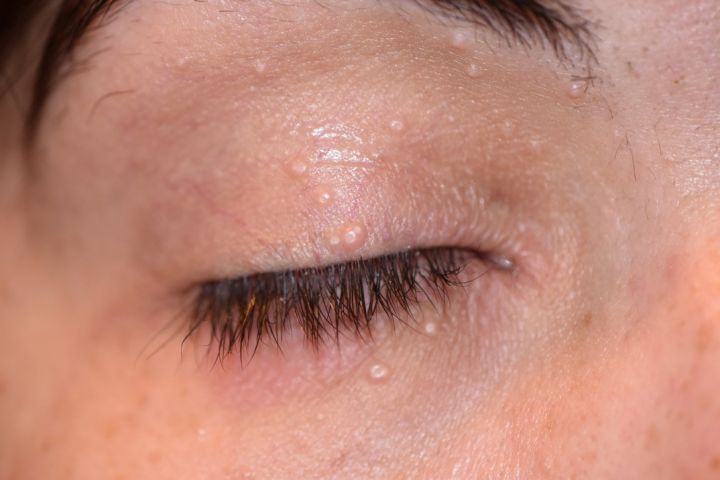

Molluscum contagiosum is a common viral skin infection caused by the molluscum contagiosum virus (MCV), a poxvirus. On the eyelids and periocular skin, it presents as small, flesh-colored, dome-shaped papules with a characteristic central umbilication, typically 2–5 mm in diameter. Lesions may be single or multiple. The condition is most common in children, immunocompromised individuals, and adults who acquire it through skin-to-skin contact.
Ocular significance: Periocular molluscum lesions located at or near the lid margin may shed viral particles onto the ocular surface, causing a chronic follicular conjunctivitis that is often misdiagnosed as allergic or viral conjunctivitis. The conjunctivitis will not resolve until the eyelid lesions are treated. Any patient with unexplained unilateral chronic follicular conjunctivitis should have the eyelid margins examined carefully for molluscum lesions.
Diagnosis is clinical based on the characteristic umbilicated appearance. Histology (if performed) shows eosinophilic intracytoplasmic inclusions — Henderson-Paterson bodies — in the epidermal keratinocytes.
Treatment options:
- Curettage — simple removal of the central umbilicated plug; effective and widely used; topical anesthetic used in children
- Cryotherapy — liquid nitrogen application to individual lesions; may require multiple treatments
- Trichloroacetic acid (TCA) — chemical ablation of individual lesions with a fine applicator
- Observation — lesions resolve spontaneously in 6–18 months in immunocompetent individuals; appropriate for asymptomatic lesions remote from the lid margin
Lid margin lesions causing follicular conjunctivitis should be treated promptly. Immunocompromised patients may develop extensive or treatment-refractory molluscum requiring systemic management.
Malignant Eyelid Lesions
Malignant eyelid tumors are predominantly epithelial in origin. The eyelid receives intense cumulative UV exposure — particularly the lower lid and medial canthus — and harbors both sebaceous glands and melanocytes, giving rise to a broad range of malignancies. The four most clinically important are basal cell carcinoma (most common), sebaceous carcinoma, squamous cell carcinoma, and melanoma.
General principles of management:
- All suspicious lesions are biopsied before definitive excision — tissue diagnosis drives surgical planning
- Margin-controlled excision (Mohs or frozen section) achieves the lowest recurrence rates for periocular malignancies
- Reconstruction is planned by Dr. Brown at the time of excision; defect size and location determine the technique (direct closure, advancement flap, rotation flap, full-thickness graft, or staged Hughes tarsoconjunctival flap)
- Sentinel lymph node biopsy is considered for high-risk squamous cell carcinoma, melanoma, and Merkel cell carcinoma
Red flags for malignancy: loss of lashes (madarosis), induration or firmness beyond the visible lesion, irregular or pearly border, telangiectatic vessels, ulceration, recurrence after treatment, or any lesion that bleeds spontaneously.
Basal Cell Carcinoma


Basal cell carcinoma (BCC) is the most common eyelid malignancy, accounting for approximately 90% of all eyelid cancers. It arises from basal keratinocytes of the epidermis and is strongly associated with cumulative UV exposure, fair skin, and immunosuppression. The lower eyelid accounts for ~50% of cases, followed by the medial canthus (~25%), upper eyelid (~15%), and lateral canthus (~10%).
Clinical subtypes:
- Nodular BCC (most common) — pearly or translucent nodule with telangiectatic vessels and a rolled, indurated border; may ulcerate centrally (“rodent ulcer”)
- Morpheaform (sclerosing) BCC — flat, waxy, scar-like plaque with ill-defined margins; most aggressive subtype, frequently underestimated clinically; requires widest surgical margins
- Superficial BCC — flat, erythematous plaque; more common on the trunk; less frequent on the eyelid
Surgical management: Mohs micrographic surgery with same-day oculoplastic reconstruction is the gold standard for periocular BCC. Mohs achieves the highest cure rate (5-year recurrence <1% for primary BCC) with the greatest tissue preservation — critical in the eyelid where even a few millimeters matter for function. For nodular BCC of the lower lid not involving the lid margin, wide local excision with frozen-section margin control is an alternative.
BCC is locally destructive but rarely metastasizes (<0.1%). Orbital invasion, though uncommon, can occur with neglected medial canthal BCC and may require orbital exenteration. Hedgehog pathway inhibitors (vismodegib, sonidegib) are used for locally advanced or metastatic BCC not amenable to surgery.

Squamous Cell Carcinoma

Squamous cell carcinoma (SCC) is the second most common eyelid malignancy, accounting for ~5% of eyelid cancers. It arises from keratinocytes of the epidermis and has a significantly higher metastatic potential than BCC — regional lymph node metastasis occurs in 1–24% of periocular SCC depending on subtype, depth, and location.
Risk factors: cumulative UV exposure, actinic keratosis (precursor lesion), immunosuppression (solid organ transplant recipients have a dramatically increased risk), xeroderma pigmentosum, chronic inflammation or scarring, and prior radiation therapy.
Clinical appearance: SCC often arises within an actinic keratosis and presents as an indurated, erythematous, scaly plaque that may ulcerate. Unlike BCC, the border tends to be less well-defined and the lesion may feel firm or fixed to deeper structures. The lower lid and lid margin are common sites.
High-risk features that increase recurrence and metastasis risk: perineural invasion, tumor thickness >2 mm, poorly differentiated histology, recurrent lesion, immunosuppressed host, and location at the lid margin or medial canthus. High-risk periocular SCC warrants sentinel lymph node biopsy or elective parotid/neck imaging.
Treatment: Mohs surgery with same-day reconstruction is preferred for primary periocular SCC. Wide local excision with frozen-section control is an alternative. Adjuvant radiation therapy is used for perineural invasion, positive margins that cannot be cleared surgically, or regional nodal disease. Anti-PD-1 therapy (cemiplimab) is approved for locally advanced or metastatic SCC not amenable to surgery or radiation.
Melanoma

Cutaneous melanoma of the eyelid is rare, accounting for ~1% of eyelid malignancies, but carries the highest mortality of all periocular skin cancers. It arises from melanocytes in the epidermis and may occur de novo or within a pre-existing nevus. The most common subtype on the eyelid is lentigo maligna melanoma (arising in a slowly enlarging, irregularly pigmented macule in sun-damaged skin of older patients), followed by superficial spreading and nodular melanoma.
Diagnosis: The “ABCDE” criteria apply: Asymmetry, Border irregularity, Color variation (multiple shades of brown, black, red, or white), Diameter >6 mm, and Evolution (change over time). Amelanotic melanoma lacks pigment and can mimic BCC or SCC — a high index of suspicion is required. Dermoscopy aids clinical assessment. Incisional or excisional biopsy with pathologic staging (Breslow depth, Clark level, mitotic rate, ulceration) is required before definitive surgery.
Treatment: Wide local excision with 5–10 mm margins (depending on Breslow depth) and sentinel lymph node biopsy for lesions >0.8 mm or with high-risk features. Lentigo maligna at the lid margin presents a reconstructive challenge because adequate margins may require full-thickness eyelid excision. Adjuvant systemic therapy (BRAF/MEK inhibitors for BRAF-mutant melanoma, anti-PD-1 immunotherapy) is used for high-risk or metastatic disease.
Sebaceous Gland Carcinoma


Sebaceous gland carcinoma (SGC) is the third most common eyelid malignancy in Western populations and the second most common in Asian populations. It arises from meibomian glands (tarsal plate), glands of Zeis (lash follicles), or sebaceous glands of the caruncle. The upper eyelid is involved twice as often as the lower eyelid — reflecting the greater number and size of meibomian glands in the upper tarsus.
SGC is notorious for masquerading as benign conditions. The most common mimics are:
- Recurrent chalazion — most dangerous masquerade; any chalazion recurring after proper I&C should be biopsied
- Chronic blepharitis or meibomian gland dysfunction
- Unilateral conjunctivitis that fails antibiotic treatment
A key feature distinguishing SGC from BCC is its ability to spread intraepithelially (pagetoid spread) throughout the conjunctival epithelium and skin without forming a discrete mass, making clinical margins unreliable. This also explains why it can present as chronic, diffuse eyelid erythema with madarosis (lash loss) — a presentation easily attributed to blepharitis for months or years.
Diagnosis: Full-thickness eyelid biopsy (including conjunctiva) and map biopsies of the conjunctiva to assess the extent of pagetoid spread. Immunohistochemistry (EMA, adipophilin, androgen receptor) confirms sebaceous differentiation. SGC is associated with Muir-Torre syndrome (MLH1 or MSH2 germline mutations) — microsatellite instability testing and oncology referral are appropriate, especially in patients under 60.
Treatment: Wide local excision with frozen-section control of all margins, including conjunctival margins if pagetoid spread is present. Sentinel lymph node biopsy is appropriate. Exenteration may be required for orbital invasion or extensive pagetoid spread. Adjuvant radiation is used for positive margins or regional nodal disease. The 5-year disease-specific mortality is ~10–20%.
Schedule a Consultation
Contact us to discuss your concerns and learn about treatment options.
Related Conditions
Blepharoplasty
Upper and lower eyelid blepharoplasty ("eye lift") — cosmetic and functional correction of excess eyelid skin and fat.
Learn more →Orbital Tumors
Diagnosis and surgical management of orbital tumors and masses — adult and pediatric, benign and malignant.
Learn more →Infections
Medical and surgical management of eyelid and orbital infections — preseptal and orbital cellulitis, dacryocystitis, herpes zoster, and more.
Learn more →